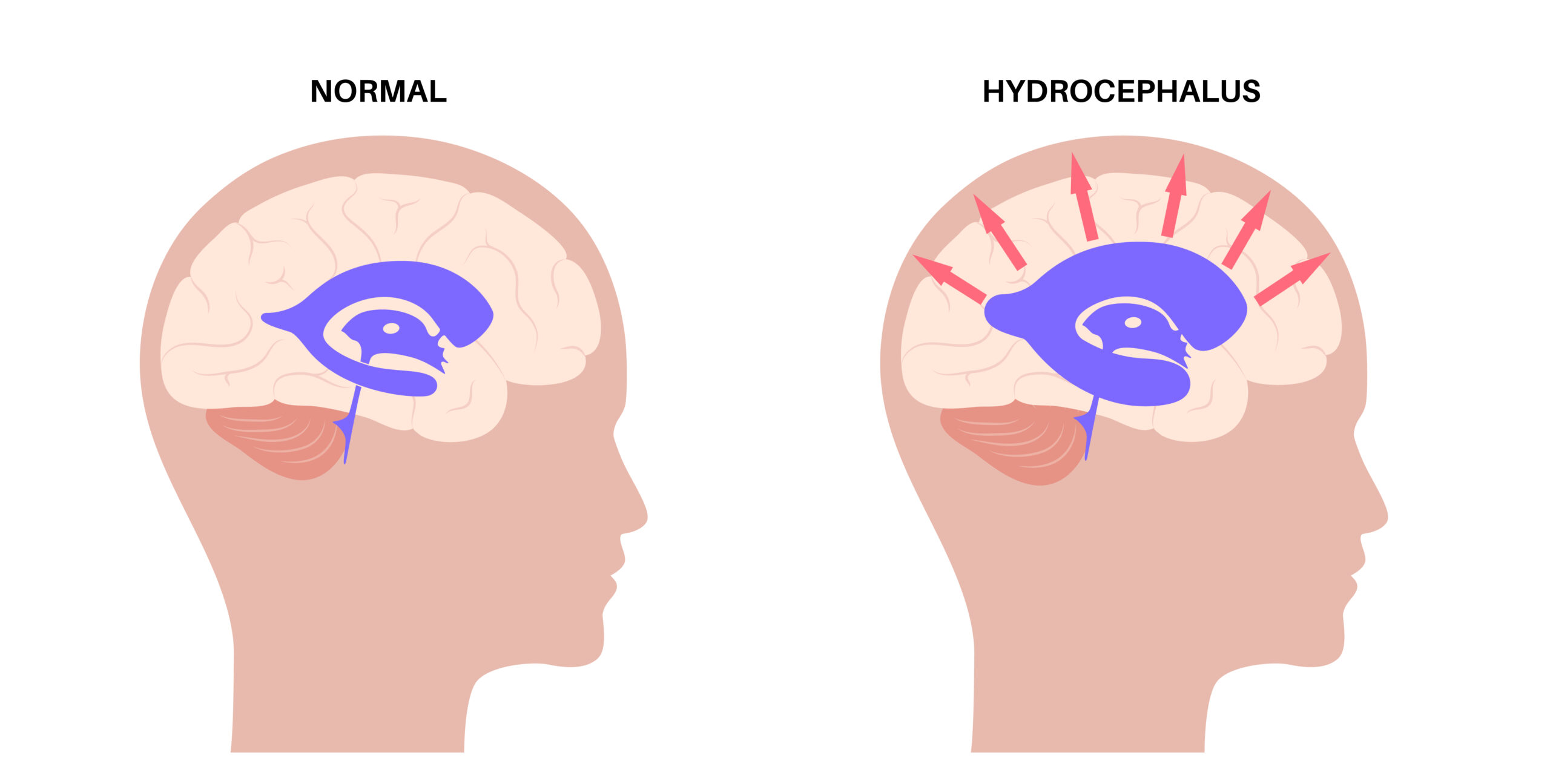
How Can Physical Therapy Help Normal Pressure Hydrocephalus?
Normal Pressure Hydrocephalus (NPH) is a neurological condition where excess cerebrospinal fluid builds up in the brain’s ventricles, leading to a classic triad of symptoms:
- Gait disturbance (often described as a “magnetic” or shuffling walk)
- Cognitive decline
- Urinary incontinence
Although medical treatment, most commonly a shunt procedure, is often necessary, physical therapy plays a critical role in improving mobility, safety, and overall quality of life.
Why Physical Therapy Matters for NPH
The most noticeable and disabling symptom of NPH is difficulty walking. Patients often experience:
- Slow, short steps
- Poor balance
- Difficulty initiating movement
- Frequent falls
Physical therapy directly targets these impairments, helping patients regain independence and confidence.
Key Ways Physical Therapy Helps
1. Gait Training
One of the primary goals is to improve walking ability.
Therapists focus on:
- Increasing step length and walking speed
- Practicing proper foot clearance
- Improving rhythm and coordination
Benefit: Patients often move from a shuffling gait to a more natural walking pattern.
2. Balance and Fall Prevention
Balance deficits are a major concern with NPH.
Therapy may include:
- Static and dynamic balance exercises
- Weight-shifting drills
- Dual-task training (walking while thinking or talking)
Benefit: Reduced fall risk and increased safety at home and in the community.
3. Strength Training
Weakness, especially in the legs, can worsen mobility issues.
Programs typically target:
- Quadriceps
- Glutes
- Core muscles
Benefit: Stronger muscles support better posture, walking, and transfers (like getting up from a chair).
4. Functional Mobility Training
This focuses on everyday movements, such as:
- Sit-to-stand transitions
- Turning and changing direction
- Getting in and out of bed
Benefit: Improved independence with daily activities.
5. Assistive Device Training
Many patients benefit from tools like:
- Walkers
- Canes
A physical therapist ensures:
- Proper fit
- Safe usage
- Progression as the patient improves
Benefit: Increased confidence and reduced fall risk.
6. Post-Shunt Rehabilitation
After a shunt procedure, physical therapy becomes even more important.
Therapists help patients:
- Re-learn improved movement patterns
- Take advantage of symptom relief
- Progress activity safely
Benefit: Maximizes the effectiveness of surgical treatment.
What Does a Typical PT Program Look Like?
A personalized program may include:
- 2–3 sessions per week initially
- A structured home exercise program
- Ongoing reassessment of gait and balance
Treatment is highly individualized, depending on severity and response to medical care.
Can Physical Therapy Cure NPH?
Physical therapy does not cure NPH, but it is one of the most effective ways to:
- Improve mobility
- Reduce falls
- Enhance independence
- Support recovery after medical treatment
Think of it as a critical piece of the overall management plan.
When Should Someone Start Physical Therapy?
Early intervention is key. You should consider PT if:
- Walking becomes slower or more unstable
- There are recent falls or near-falls
- A diagnosis of NPH has been made
- A shunt procedure is planned or completed
Normal Pressure Hydrocephalus can significantly impact daily life, but with the right combination of medical care and targeted physical therapy, many patients see meaningful improvements. Physical therapy helps bridge the gap between diagnosis and real-world function, turning clinical progress into safer walking, better balance, and greater independence. If you have questions about how physical therapy can help with NPH, contact our office at 480-719-8000.